Case of the Week
Case Brief
Case Brief
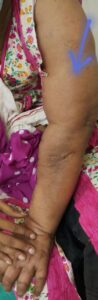
A female aged 53yrs presents to the Oncology OPD of your hospital complaining of a large, painful, fungating mass on her left breast with massive swelling of her entire left upper limb. She narrates that the lump was initially the size of a lemon, painless but progressively increased in size over 8 months leading to a painful ulcerative lesion in the skin overlying the lump, which eventually ruptured. Her left arm began to swell up over the last 3 months.
On examination, you palpate a hard lump approx. 8cm × 8cm almost involving the entire left breast mass including the nipple areolar complex. It appears to be fixed to the overlying skin and the underlying pectoralis major. There is an obvious skin ulcer overlying the lump, with mucopurulent discharge. There are no palpable skin nodules. Superficial veins of the left chest wall are engorged. Left axillary examination reveals a hard painless lump about 3cm × 4cm involving anterior & central lymph nodes. The right breast and axilla are unremarkable. No lymph nodes are palpable on either side of the neck. There is painless pitting oedema in her left upper limb.
She is on medication for diabetes mellitus and ischaemic heart disease for the last 10 years. She is post menopausal, a mother of two children, has no addictions or family history of malignancy.
You end up with a clinical provisional diagnosis of carcinoma of the left breast.
Q1. What is your clinical staging of the disease? Explain why.
Q2. Explain the arm swelling.
Q3. How will you proceed to confirm your diagnosis?
Q4. What special test would you advice for classifying the disease? How would it affect the treatment?
Q5. What would be the most appropriate course of management, in case of an invasive carcinoma of the left breast without distal metastasis? (Explain with rationale)
Q6. What is the 1st line Chemotherapy regimen currently recommended for carcinoma of breast?
A female aged 53yrs presents to the Oncology OPD of your hospital complaining of a large, painful, fungating mass on her left breast with massive swelling of her entire left upper limb. She narrates that the lump was initially the size of a lemon, painless but progressively increased in size over 8 months leading to a painful ulcerative lesion in the skin overlying the lump, which eventually ruptured. Her left arm began to swell up over the last 3 months.
On examination, you palpate a hard lump approx. 8cm × 8cm almost involving the entire left breast mass including the nipple areolar complex. It appears to be fixed to the overlying skin and the underlying pectoralis major. There is an obvious skin ulcer overlying the lump, with mucopurulent discharge. There are no palpable skin nodules. Superficial veins of the left chest wall are engorged. Left axillary examination reveals a hard painless lump about 3cm × 4cm involving anterior & central lymph nodes. The right breast and axilla are unremarkable. No lymph nodes are palpable on either side of the neck. There is painless pitting oedema in her left upper limb.
She is on medication for diabetes mellitus and ischaemic heart disease for the last 10 years. She is post menopausal, a mother of two children, has no addictions or family history of malignancy.
You end up with a clinical provisional diagnosis of carcinoma of the left breast.
Q1. What is your clinical staging of the disease? Explain why.
Q2. Explain the arm swelling.
Q3. How will you proceed to confirm your diagnosis?
Q4. What special test would you advice for classifying the disease? How would it affect the treatment?
Q5. What would be the most appropriate course of management, in case of an invasive carcinoma of the left breast without distal metastasis? (Explain with rationale)
Q6. What is the 1st line Chemotherapy regimen currently recommended for carcinoma of breast?
Submit Answers
Submit Answers